慢性前列腺炎/慢性骨盆疼痛綜合症:修订间差异
无编辑摘要 |
|||
| 第37行: | 第37行: | ||
===食物過敏=== |
===食物過敏=== |
||
有證據表明,食物過敏和不耐受可能在慢性前列腺炎/慢性骨盆疼痛綜合症方面起了加重病情的作用,也許是肥大細胞的介導機制所致。也有一些證據表明在一些患者的泌尿系統慢性盆腔疼痛綜合症(如間質性膀胱炎/膀胱疼痛綜合症和慢性前列腺炎/慢性骨盆疼痛綜合症 )與{{le|麩質不耐|Non-celiac_gluten_sensitivity}}有關<ref name=Catassi2015>{{cite journal|author= Catassi C|title=Gluten Sensitivity|year=2015|journal=Ann Nutr Metab|volume=67 Suppl 2|pages=16–26|doi=10.1159/000440990|url= http://www.karger.com/Article/FullText/440990 |
有證據表明,食物過敏和不耐受可能在慢性前列腺炎/慢性骨盆疼痛綜合症方面起了加重病情的作用,也許是肥大細胞的介導機制所致。也有一些證據表明在一些患者的泌尿系統慢性盆腔疼痛綜合症(如間質性膀胱炎/膀胱疼痛綜合症和慢性前列腺炎/慢性骨盆疼痛綜合症 )與{{le|麩質不耐|Non-celiac_gluten_sensitivity}}有關<ref name=Catassi2015>{{cite journal|author= Catassi C|title=Gluten Sensitivity|year=2015|journal=Ann Nutr Metab|volume=67 Suppl 2|pages=16–26|doi=10.1159/000440990|url= http://www.karger.com/Article/FullText/440990 |
||
|pmid= 26605537|type=Review}}</ref><ref name="pmid23204003">{{cite journal |vauthors=Rostami K, Hogg-Kollars S |title=A Patient's Journey. Non-coeliac gluten sensitivity |journal=BMJ |volume=345 |issue= |pages=e7982 |year=2012 |pmid=23204003 |doi= |url=}}</ref><ref>{{cite web |url=http://www.chronicprostatitis.com/gluten-and-chronic-prostatitis-cpps/ |title=Gluten and CP/CPPS |work=Prostatitis Network |accessdate=2016-03-16 }}</ref>。因此,患者通過識別問題食品然後把其从飲食中消除可能對減輕症狀有幫助。這方面的研究較为缺乏 |
|pmid= 26605537|type=Review}}</ref><ref name="pmid23204003">{{cite journal |vauthors=Rostami K, Hogg-Kollars S |title=A Patient's Journey. Non-coeliac gluten sensitivity |journal=BMJ |volume=345 |issue= |pages=e7982 |year=2012 |pmid=23204003 |doi= |url=}}</ref><ref>{{cite web |url=http://www.chronicprostatitis.com/gluten-and-chronic-prostatitis-cpps/ |title=Gluten and CP/CPPS |work=Prostatitis Network |accessdate=2016-03-16 }}</ref>。因此,患者通過識別問題食品然後把其从飲食中消除可能對減輕症狀有幫助。這方面的研究較为缺乏。 |
||
==診斷== |
|||
沒有確切的對慢性前列腺炎/慢性骨盆疼痛綜合症的診斷測試。這是一種所知甚少的病症。儘管它佔所有前列腺炎診斷的90%-95%<ref name="pmid16409145">{{cite journal |author=Habermacher GM, Chason JT, Schaeffer AJ |title=Prostatitis/chronic pelvic pain syndrome |journal=Annu. Rev. Med. |volume=57 |issue= |pages=195–206 |year=2006 |pmid=16409145 |doi=10.1146/annurev.med.57.011205.135654|last2=Chason |last3=Schaeffer }}</ref>。它可在任何年齡的男性中被發現,35-45歲为男性發病高峰<ref name="shosk1">{{cite book |title=Chronic Prostatitis/Chronic Pelvic Pain Syndrome |pages=171 |author=Daniel Shoskes |url=http://books.google.com/?id=tHZ9thCt4skC&pg=PT171&lpg=PT171 |isbn=1-934115-27-4 |year=2008 |publisher=Humana Press}}</ref>。慢性前列腺炎/慢性骨盆疼痛綜合症可以根據前列腺液分泌物中的膿細胞水平,分为炎症(分類ⅢA)或是非炎症(分類ⅢB),但這些子類別在臨床上用途有限。在分類為炎症的情況下,尿液、精液、其它從前列腺流出來的液體包含膿細胞(死去的白血細胞或白細胞);而分類為非炎症的情況下,並无發現膿細胞存在。最近的研究質疑分類Ⅲa和Ⅲb之間的區別,因為如果膿細胞和更細微的跡象(如所測量的[[细胞因子]])被忽略,這兩類都表明是炎症<ref name="A Pontari-2002">{{Cite journal | last1 = A Pontari | first1 = M. | title = Inflammation and anti-inflammatory therapy in chronic prostatitis | journal = Urology | volume = 60 | issue = 6 Suppl | pages = 29–33; discussion 33–4 |date=Dec 2002 | doi = 10.1016/S0090-4295(02)02381-6| pmid = 12521589 }}</ref>。 |
|||
==參考資料== |
==參考資料== |
||
2016年8月1日 (一) 14:20的版本
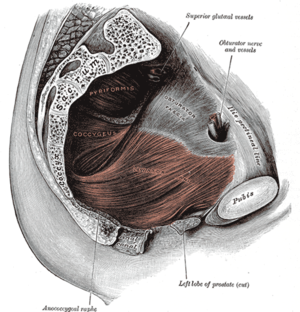
| 慢性非細菌性前列腺炎 (Chronic nonbacterial prostatitis) | |
|---|---|
 | |
| 类型 | urologic chronic pelvic pain syndrome[*]、慢性前列腺炎 |
| 分类和外部资源 | |
| 醫學專科 | 泌尿外科 |
| ICD-10 | N41.1 |
| ICD-9-CM | 601.1 |
| DiseasesDB | 10801 |
| MedlinePlus | 000524 |
| eMedicine | article/437745 |
| MeSH | D011472 |
慢性非细菌性前列腺炎(Chronic nonbacterial prostatitis)或慢性前列腺炎/慢性骨盆疼痛綜合症(chronic prostatitis/chronic pelvic pain syndrome )是男性盆腔疼痛的一種狀態,並且應該與其他类型的前列腺炎區分,如慢性細菌性前列腺炎和急性細菌性前列腺炎[1][2]。這種情況以前被稱為前列腺疼痛(prostatodynia)。
症狀
慢性前列腺炎/慢性骨盆疼痛綜合徵的主要特徵是骨盆骨盆或會陰疼痛,而沒有尿路感染的跡象[3],並持續超過3個月[4],此乃關鍵症狀。它的症狀可能会时好轉时恶化。痛楚的程度可以從輕微的,以至使人虛弱。痛楚可散發至背部和直腸,令人坐下时感到不舒服。可於會陰、睾丸、陰莖前端、恥骨或膀胱區上感到痛楚[5]。排尿困難、關節痛、肌肉痛、不明原因的乏力、腹痛、陰莖不斷灼痛也是時常会出現的症狀。尿頻和尿急可能是暗示是患上間質性膀胱炎(膀胱而不是前列腺有炎症)。由神經和肌肉介導的射精後疼痛,是其一大特點[6],用以把慢性前列腺炎/慢性骨盆疼痛綜合症患者與良性前列腺增生症或正常男性區分。有些患者報告說自己性慾低下、性功能障礙和勃起困難。
原因
神經、壓力和荷爾蒙
慢性前列腺炎/慢性骨盆疼痛綜合症是免疫、神經和內分泌系統與心理因素之間的相互作用導致[7]。該病背後的理論包括壓力令下丘脑-垂体-肾上腺轴功能失調和腎上腺皮質激素(內分泌)異常[8][9]、神經源性炎症[10][11][12]、肌筋膜疼痛症候群[13][14]。在後兩類,是由於過去的創傷、感染或焦慮性格導致局部神經系統的失調,慢性無意識地繃緊骨盆(受神經細胞釋放物質(如物質P)的調節)亦会導致炎症。前列腺(和泌尿生殖道其它部分:膀胱、尿道、睾丸)亦能因長期活化在骨盆神經端部的肥大細胞而發炎。類似壓力誘發的生殖泌尿炎症已經在其他哺乳動物實驗中發現[15]。然而,前列腺炎組織學檢查與國立衛生研究院的慢性前列腺炎症狀指數之間沒有關聯[16]。
細菌感染學說曾在這一領域長時間佔居主導地位,但於2003年在華盛頓大學由李博士(Dr Lee)和理查德·伯傑(Professor Richard Berger)教授帶領的研究顯示細菌感染並不重要。該研究發現,三分之一正常男性或患者前列腺都有類近的細菌數量[17]。這一觀點得到了西北大學泌尿外科主任和教授安東尼·謝弗博士(Dr Anthony Schaeffer)贊同,在2003年的泌尿外科雜誌中,他指出「這些數據表明,細菌在慢性骨盆疼痛綜合症的病情發展中並不扮演一個顯著角色[18] 。」;並在一年後與他的同事發表他的研究,顯示抗生素對慢性前列腺炎/慢性骨盆疼痛綜合症基本上是無用的[19][20]。由於這些研究報告的發表,研究重點已經從感染轉移到神經肌肉、行為、心理和遺傳去研究UCPPS病因(UCPPS:慢性前列腺炎/慢性骨盆疼痛綜合症、間質性膀胱炎/膀胱疼痛綜合症),其中強調下尿路和其他生理系統之間的相互作用[21]。現在的研究把UCPPS視為一種全身性疾病[21]。為佐證這項提議,2005年的研究表明,壓力是與第三類前列腺炎(慢性前列腺炎/慢性骨盆疼痛綜合症)相關的[22]。
與間質性膀胱炎/膀胱疼痛綜合症重疊
一些研究人員認為,慢性骨盆疼痛綜合症是間質性膀胱炎/膀胱疼痛綜合症的一種形式。2007年,美国国立糖尿病消化与肾病研究所开始把間質性膀胱炎/膀胱疼痛綜合症和慢性前列腺炎/慢性骨盆疼痛綜合症組合,統稱泌尿系統慢性盆腔疼痛綜合症(Urologic Chronic Pelvic Pain Syndromes )。對間質性膀胱炎/膀胱疼痛綜合症有效的治療,如槲皮素[23],在慢性前列腺炎/慢性骨盆疼痛綜合症中同樣有一些療效[24]。最近的研究集中在基因組學和蛋白质组学方面的相關條件[25]。
患者可能在膀胱充盈時出現疼痛,這也是膀胱疼痛綜合症的典型症狀[26]。
氣候
環境溫度在病情上也扮演一个角色。患者很多时候会報告説寒冷引起症狀加重,熱力則很多时候会被報告説改善症狀[27]。这則顯得寒冷是可以引發導致慢性前列腺炎/慢性骨盆疼痛綜合症的過程的因素之一[28]。寒冷也導致症狀加重和復發[28][29]。一項調查表明,居住在寒冷氣候下的芬蘭北部的男性前列腺炎症狀的發生率比在世界其它地方報告的數字高[30]。
食物過敏
有證據表明,食物過敏和不耐受可能在慢性前列腺炎/慢性骨盆疼痛綜合症方面起了加重病情的作用,也許是肥大細胞的介導機制所致。也有一些證據表明在一些患者的泌尿系統慢性盆腔疼痛綜合症(如間質性膀胱炎/膀胱疼痛綜合症和慢性前列腺炎/慢性骨盆疼痛綜合症 )與麩質不耐有關[31][32][33]。因此,患者通過識別問題食品然後把其从飲食中消除可能對減輕症狀有幫助。這方面的研究較为缺乏。
診斷
沒有確切的對慢性前列腺炎/慢性骨盆疼痛綜合症的診斷測試。這是一種所知甚少的病症。儘管它佔所有前列腺炎診斷的90%-95%[34]。它可在任何年齡的男性中被發現,35-45歲为男性發病高峰[35]。慢性前列腺炎/慢性骨盆疼痛綜合症可以根據前列腺液分泌物中的膿細胞水平,分为炎症(分類ⅢA)或是非炎症(分類ⅢB),但這些子類別在臨床上用途有限。在分類為炎症的情況下,尿液、精液、其它從前列腺流出來的液體包含膿細胞(死去的白血細胞或白細胞);而分類為非炎症的情況下,並无發現膿細胞存在。最近的研究質疑分類Ⅲa和Ⅲb之間的區別,因為如果膿細胞和更細微的跡象(如所測量的细胞因子)被忽略,這兩類都表明是炎症[36]。
參考資料
- ^ Schaeffer, A. J.; Datta, N. S.; Fowler Jr, J. E.; Krieger, J. N.; Litwin, M. S.; Nadler, R. B.; Nickel, J. C.; Pontari, M. A.; Shoskes, D. A.; Zeitlin, S. I.; Hart, C.; Chronic Prostatitis Collaborative Research Network. Overview summary statement. Diagnosis and management of chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS). Urology. 2002, 60 (6 Suppl): 1–4. PMID 12521576. doi:10.1016/S0090-4295(02)01979-9.
- ^ Holt JD1 et al. Common Questions About Chronic Prostatitis. Am Fam Physician. 2016 Feb 15;93(4):290-6. PMID 26926816
- ^ Schaeffer AJ. Epidemiology and evaluation of chronic pelvic pain syndrome in men. Int J Antimicrob Agents. 2007, 31: S108–11. PMID 18164597. doi:10.1016/j.ijantimicag.2007.08.027.
- ^ Luzzi GA. Chronic prostatitis and chronic pelvic pain in men: aetiology, diagnosis and management. Journal of the European Academy of Dermatology and Venereology : JEADV. 2002, 16 (3): 253–6. PMID 12195565. doi:10.1046/j.1468-3083.2002.00481.x.
- ^ Clemens, J Quentin; Meenan, Richard T; O'Keeffe Rosetti, Maureen C; Gao, Sara Y; Calhoun, Elizabeth A. Incidence and clinical characteristics of National Institutes of Health type III prostatitis in the community. J Urol. Dec 2005, 174 (6): 2319–22. PMID 16280832. doi:10.1097/01.ju.0000182152.28519.e7.
- ^ Shoskes DA, Landis JR, Wang Y, Nickel JC, Zeitlin SI, Nadler R; Landis; Wang; Nickel; Zeitlin; Nadler; Chronic Prostatitis Collaborative Research Network Study Group. Impact of post-ejaculatory pain in men with category III chronic prostatitis/chronic pelvic pain syndrome. J. Urol. August 2004, 172 (2): 542–7. PMID 15247725. doi:10.1097/01.ju.0000132798.48067.23.
- ^ Pontari MA, Ruggieri MR; Ruggieri. Mechanisms in prostatitis/chronic pelvic pain syndrome. J. Urol. May 2008, 179 (5 Suppl): S61–7. PMID 18405756. doi:10.1016/j.juro.2008.03.139.
- ^ Anderson RU, Orenberg EK, Chan CA, Morey A, Flores V; Orenberg; Chan; Morey; Flores. Psychometric Profiles and Hypothalamic-Pituitary-Adrenal Axis Function in Men With Chronic Prostatitis/Chronic Pelvic Pain Syndrome. J Urol. 2008, 179 (3): 956–60. PMC 2694575
 . PMID 18207189. doi:10.1016/j.juro.2007.10.084.
. PMID 18207189. doi:10.1016/j.juro.2007.10.084.
- ^ Dimitrakov J, Joffe HV, Soldin SJ, Bolus R, Buffington CA, Nickel JC; Joffe; Soldin; Bolus; Buffington; Nickel. Adrenocortical Hormone Abnormalities in Men with Chronic Prostatitis/Chronic Pelvic Pain Syndrome. Urology. 2008, 71 (2): 261–266. PMC 2390769
 . PMID 18308097. doi:10.1016/j.urology.2007.09.025.
. PMID 18308097. doi:10.1016/j.urology.2007.09.025.
- ^ Theoharides TC, Cochrane DE; Cochrane. Critical role of mast cells in inflammatory diseases and the effect of acute stress. J. Neuroimmunol. 2004, 146 (1–2): 1–12. PMID 14698841. doi:10.1016/j.jneuroim.2003.10.041.
- ^ Theoharides TC, Kalogeromitros D; Kalogeromitros. The critical role of mast cells in allergy and inflammation. Ann. N. Y. Acad. Sci. 2006, 1088: 78–99. Bibcode:2006NYASA1088...78T. PMID 17192558. doi:10.1196/annals.1366.025.
- ^ Sant GR, Kempuraj D, Marchand JE, Theoharides TC; Kempuraj; Marchand; Theoharides. The mast cell in interstitial cystitis: role in pathophysiology and pathogenesis. Urology. 2007, 69 (4 Suppl): 34–40. PMID 17462477. doi:10.1016/j.urology.2006.08.1109.
- ^ Anderson RU, Wise D, Sawyer T, Chan C; Wise; Sawyer; Chan. Integration of myofascial trigger point release and paradoxical relaxation training treatment of chronic pelvic pain in men. J. Urol. 2005, 174 (1): 155–60. PMID 15947608. doi:10.1097/01.ju.0000161609.31185.d5.
- ^ Anderson RU, Wise D, Sawyer T, Chan CA; Wise; Sawyer; Chan. Sexual dysfunction in men with chronic prostatitis/chronic pelvic pain syndrome: improvement after trigger point release and paradoxical relaxation training. J. Urol. 2006, 176 (4 Pt 1): 1534–8; discussion 1538–9. PMID 16952676. doi:10.1016/j.juro.2006.06.010.
- ^ Alexacos N, Pang X, Boucher W, Cochrane DE, Sant GR, Theoharides TC; Pang; Boucher; Cochrane; Sant; Theoharides. Neurotensin mediates rat bladder mast cell degranulation triggered by acute psychological stress. Urology. 1999, 53 (5): 1035–40. PMID 10223502. doi:10.1016/S0090-4295(98)00627-X.
- ^ Nickel JC, Roehrborn CG, O'leary MP, Bostwick DG, Somerville MC, Rittmaster RS; Roehrborn; O'Leary; Bostwick; Somerville; Rittmaster. Examination of the relationship between symptoms of prostatitis and histological inflammation: baseline data from the REDUCE chemoprevention trial. J. Urol. 2007, 178 (3 Pt 1): 896–900; discussion 900–1. PMID 17632164. doi:10.1016/j.juro.2007.05.041.
- ^ Lee JC; Muller CH; Rothman I; et al. Prostate biopsy culture findings of men with chronic pelvic pain syndrome do not differ from those of healthy controls. J. Urol. February 2003, 169 (2): 584–7; discussion 587–8. PMID 12544312. doi:10.1097/01.ju.0000045673.02542.7a (不活跃 2015-01-11).
- ^ Schaeffer AJ. Editorial: Emerging concepts in the management of prostatitis/chronic pelvic pain syndrome. J Urol. 2003, 169 (2): 597–598. PMID 12544315. doi:10.1016/S0022-5347(05)63961-4.
- ^ Alexander RB; Propert KJ; Schaeffer AJ; et al. Ciprofloxacin or tamsulosin in men with chronic prostatitis/chronic pelvic pain syndrome: a randomized, double-blind trial. Ann. Intern. Med. 2004, 141 (8): 581–9. PMID 15492337. doi:10.7326/0003-4819-141-8-200410190-00005.
- ^ Nickel JC; Downey J; Clark J; et al. Levofloxacin for chronic prostatitis/chronic pelvic pain syndrome in men: a randomized placebo-controlled multicenter trial. Urology. 2003, 62 (4): 614–7. PMID 14550427. doi:10.1016/S0090-4295(03)00583-1.
- ^ 21.0 21.1 Multi-disciplinary Approach to the Study of Chronic Pelvic Pain. NIDDK—Department of Health and Human Services. 2007 [2008-02-12].
- ^ Ullrich PM, Turner JA, Ciol M, Berger R; Turner; Ciol; Berger. Stress is associated with subsequent pain and disability among men with nonbacterial prostatitis/pelvic pain. Annals of Behavioral Medicine. 2005, 30 (2): 112–8. PMID 16173907. doi:10.1207/s15324796abm3002_3.
- ^ Theoharides, TC.; Whitmore, K.; Stanford, E.; Moldwin, R.; O'Leary, MP. Interstitial cystitis: bladder pain and beyond. Expert Opin Pharmacother. Dec 2008, 9 (17): 2979–94. PMID 19006474. doi:10.1517/14656560802519845.
- ^ Murphy, AB.; Macejko, A.; Taylor, A.; Nadler, RB. Chronic prostatitis: management strategies. Drugs. 2009, 69 (1): 71–84. PMID 19192937. doi:10.2165/00003495-200969010-00005.
- ^ Dimitrakov, J.; Dimitrakova, E. Urologic chronic pelvic pain syndrome—looking back and looking forward. Folia Med (Plovdiv). 2009, 51 (3): 42–4. PMID 19957562.
- ^ Rourke W, Khan SA, Ahmed K, Masood S, Dasgupta P, Khan MS; Khan; Ahmed; Masood; Dasgupta; Khan. Painful bladder syndrome/interstitial cystitis: aetiology, evaluation and management. Arch Ital Urol Androl. June 2014, 86 (2): 126–31. PMID 25017594. doi:10.4081/aiua.2014.2.126.
- ^ Hedelin H, Jonsson K; Jonsson. Chronic prostatitis/chronic pelvic pain syndrome: symptoms are aggravated by cold and become less distressing with age and time. Scand. J. Urol. Nephrol. 2007, 41 (6): 516–20. PMID 17853027. doi:10.1080/00365590701428517.
- ^ 28.0 28.1 Hedelin H, Jonsson K; Jonsson. Chronic abacterial prostatitis and cold exposure: an explorative study. Scand. J. Urol. Nephrol. 2007, 41 (5): 430–5. PMID 17853032. doi:10.1080/00365590701365123.
- ^ Gao DJ, Guo YS, Yu HY, Wang YJ, Cui WG; Guo; Yu; Wang; Cui. [Prevalence and related factors of prostatitis-like symptoms in young men]. Zhonghua Nan Ke Xue. December 2007, 13 (12): 1087–90. PMID 18284056 (Chinese).
- ^ Mehik A, Hellström P, Lukkarinen O, Sarpola A, Järvelin M; Hellström; Lukkarinen; Sarpola; Järvelin. Epidemiology of prostatitis in Finnish men: a population-based cross-sectional study. BJU Int. September 2000, 86 (4): 443–8. PMID 10971269. doi:10.1046/j.1464-410X.2000.00836.x.
- ^ Catassi C. Gluten Sensitivity. Ann Nutr Metab (Review). 2015,. 67 Suppl 2: 16–26. PMID 26605537. doi:10.1159/000440990.
- ^ Rostami K, Hogg-Kollars S. A Patient's Journey. Non-coeliac gluten sensitivity. BMJ. 2012, 345: e7982. PMID 23204003.
- ^ Gluten and CP/CPPS. Prostatitis Network. [2016-03-16].
- ^ Habermacher GM, Chason JT, Schaeffer AJ; Chason; Schaeffer. Prostatitis/chronic pelvic pain syndrome. Annu. Rev. Med. 2006, 57: 195–206. PMID 16409145. doi:10.1146/annurev.med.57.011205.135654.
- ^ Daniel Shoskes. Chronic Prostatitis/Chronic Pelvic Pain Syndrome. Humana Press. 2008: 171. ISBN 1-934115-27-4.
- ^ A Pontari, M. Inflammation and anti-inflammatory therapy in chronic prostatitis. Urology. Dec 2002, 60 (6 Suppl): 29–33; discussion 33–4. PMID 12521589. doi:10.1016/S0090-4295(02)02381-6.
外部連結
| |||||||||||||||||||||||||||||||||||||||||||||||||||||
